- Category
- War in Ukraine
What Your Day Looks Like as a Combat Medic in Ukraine
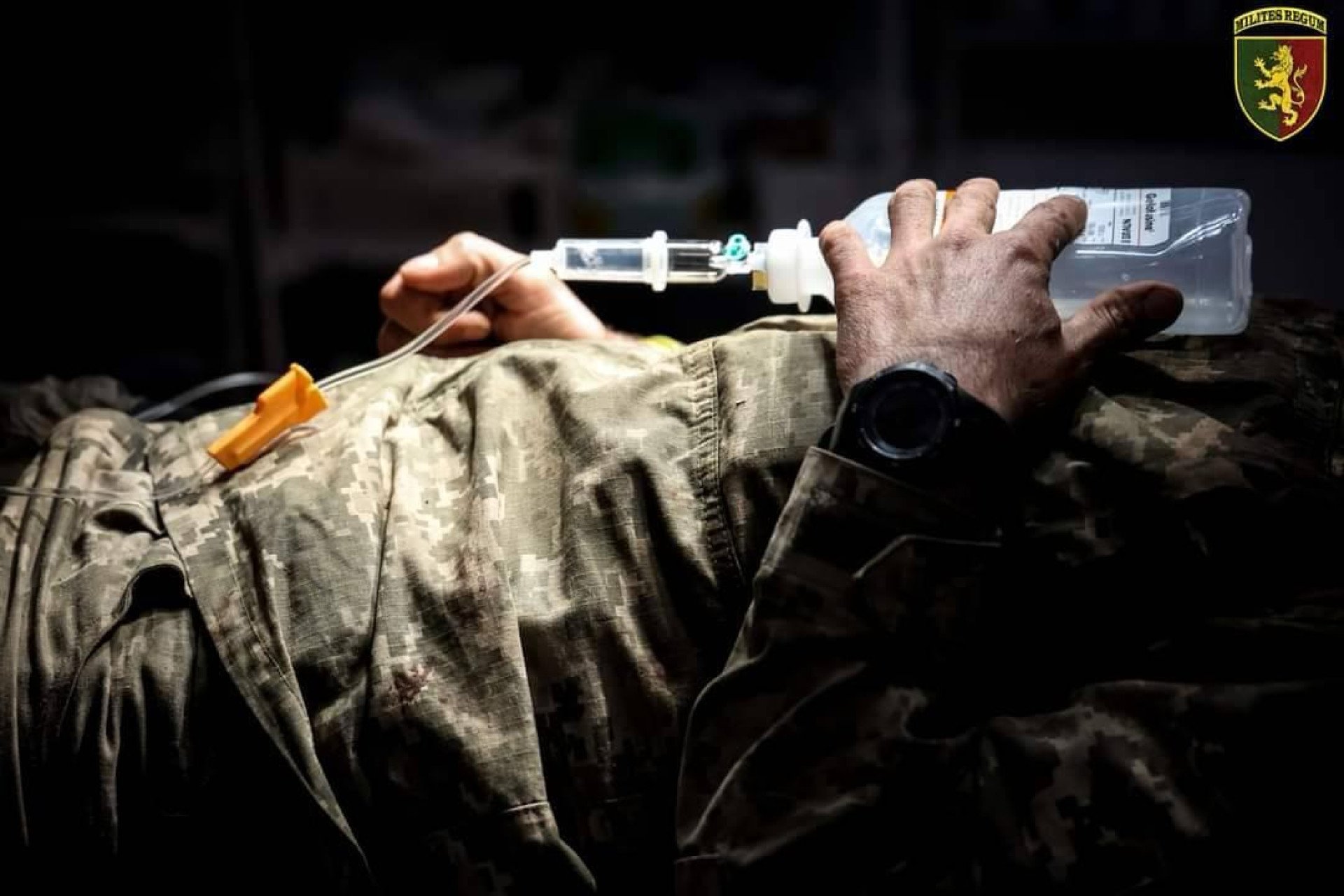
While Russia is taking lives, others are doing everything they can to save them. Every day, thousands of combat medics and doctors make their utmost effort to preserve the lives and health of Ukraine’s defenders. In evacuation vehicles, at stabilization points, and in hospitals, their mission remains unchanged—to ensure their patients survive. We spoke with four medics about the challenges they face.
The medics featured in this story shared their experiences while staying in Sweden as part of the Repower program—a project aimed at the psychological recovery of Ukrainian combat medics and doctors.
You rush toward the wounded without even turning off the engine
Vlad Ryzhkin, Driver-medic, the 128th Heavy Mechanized Brigade “Wild Field”:
My service began on February 24, 2022. For the first six months, I served in the infantry as a machine gunner. I went through a lot: evacuating the wounded from tree lines and directly from the battlefield. At that time, there were no drones. The medevac unit was interested in me, and I had noticed them too. I really wanted to join, but there were no open positions.

Since late summer 2022, I’ve been evacuating the wounded. My first mission was the hardest, the worst. I got assigned to it by chance. One of the medevac drivers arranged for me to be transferred from my unit to their team for three days.
“A paramedic will arrive with a vehicle,” he told me, “and you’ll get in and figure everything out.” But when the paramedic arrived, he didn't say, “Let’s go, we’ll try and learn.” He just rushed in: “Didn’t anyone tell you? Get ready. We already have a lot of wounded—there’s no time.”
Into the “red” zone
I jumped into the vehicle, and we received a radio request to head to a specific checkpoint. There, we were personally asked to drive into a tree line—into the “red” zone. Medevac crews operate in the “yellow” and “green” zones, but they don’t enter the “red” zone. They were directing us to a tree line—the same one where I’d been stationed back when I was in the infantry. I knew it well.
We bring you stories from the ground. Your support keeps our team in the field.
My first wounded were a father and son from the infantry. Not from my company, but still—a father and son. The son was in moderate condition, and the father was closer to critical. It was very difficult. At the time, our evacuation route stretched 47 kilometers (29 miles), and there were no proper roads.
I hadn’t taken any medical courses before that. I’d never had to do anything like this either in civilian life. Halfway there, the paramedic shouted to me, “Get inside, I need your help.”
The second time, we went back to pick up another casualty. We left the vehicle and walked to get him. It turned out someone had given us the wrong information—he was “200.” His vehicle, which had been carrying ammunition, was blown up. Someone else had already evacuated a wounded man using their pickup truck. The other one, the driver, was lying there completely burned. By then, I had already seen the dead bodies in the infantry, seen the wounded, and evacuated them—but this was still very hard.
While we were driving back, a tank crew stopped us right on the road. There was another man who was severely burned—70–80% of his body was covered in burns. We took him and transported him. And all of this—with such a long evacuation route—meant 100 kilometers (62 miles) for a round trip.
We got back, and the paramedic introduced me to everyone, telling them, “I want him to be our new driver.” The chief medical officer came out and asked, “Would you mind?” “That’s fine with me,” I said. And that was it—I stayed. As they later told me, my first day was the toughest anyone had ever had on the evacuation team.
Drone war
Before, when we were up against mortars and artillery, we worked a bit differently—we could slow down in some places, speed up in others, pull into a tree line to quickly help the patient in the vehicle. But now that’s unrealistic. Now you drive fueled purely by fear. You ask the command post what’s happening in the sky. They answer you, but they can’t tell you about “waiters”—drones lying in wait. Who could know about them? Only if you’re lucky—if a drone flew over some positions, someone heard it land somewhere and passed that information along. Then yes, we’ll sit and wait for a while.
It’s great that the guys [soldiers—ed.] now come out with anti-drone guns if we ask for help. They step out or climb into position, and when we’re driving—especially along certain positions—they all try to monitor the situation to make sure the evacuation goes smoothly. So if a drone follows us along the same logistics route, they’ll try to shoot it down.

Evacuation means you rush in and don’t even turn off the engine. I jump out, the medic runs behind me and opens the doors. The guys who are in the position help bring the wounded over. The medic grabs him. At that moment, I’m standing there with an anti-drone shotgun, monitoring what’s happening around us. As soon as the doors close behind the medic and the wounded soldier, I toss the shotgun onto the seat to my right, slam the door, and hit the gas. Then they just hold on tight in the back, and we drive as fast as possible—over hills and through potholes—pushing the vehicle to the limit.
“It’ll be okay, don’t rush”
The hardest part—and this may sound harsh—is doing your job without taking it all too close to heart.
Vlad Ryzhkin
Driver-medic, the 128th Heavy Mechanized Brigade “Wild Field”
Before, I used to take it personally, and it was really hard—I would end up in tears. It’s people you’ve been serving with in the infantry since 2022—and you’re evacuating one of them, sometimes not even wounded, but killed in action. There was one guy I knew who we evacuated four times. He was never just concussed; it was always shrapnel wounds.
What I’ll remember for the rest of my life is a man who died right in our vehicle on the way—we couldn’t get him to the hospital. We had an evacuation point, and he was brought to us—his arms and legs were broken, and he was severely wounded. We wanted to transfer him, but it was impossible. He was on soft stretchers, so we just placed them on top of ours. We set off, and, of all things, I remember that as we were driving, either “Vasilek” or something else started firing at us from our right.


Then the paramedic shouts, “Stop!” I rushed over, put on gloves, and this man said with a calm voice, “It’s hard to breathe.” “Lift him,” the paramedic said. I lifted him and saw holes in his back—later I learned there were 13, all different sizes, all across his back. I shouted, “Occlusive dressing!” The paramedic started tearing it, but it was summer, hot, and it stuck poorly, so he had to tear it with his teeth.
And this man, at that moment—probably the words that struck me most—said, “It’ll be okay, don’t worry. It’ll be okay, don’t rush.” I’ll remember that for the rest of my life. We put the occlusive dressings on him and drove off. On the way, another medic, who is currently our chief medical officer, jumped into the vehicle. Together, they worked to save the patient, giving adrenaline and helping him breathe.
I remember they shouted at me, “Stop!” I stopped so they could work. They began breathing for him, pumping him. Then they said, “It’s over.” I asked, “What do you mean? Let’s go.” The paramedic said, “It’s over,” took the patient’s dangling arm and repositioned it, repeating, “It’s over.”
I got out of the vehicle, and for the first 20–30 seconds, I don’t remember anything. I didn’t understand what was happening or where we were. I just remember walking with tears streaming down my face.
Until 2024, I hadn’t taken any medical courses—no one taught me anything at all. I learned by watching and copying others. I didn’t even approach the guys I worked with. Of course, they didn’t give me the serious cases right away. I started with what you could call simple tasks: helping a soldier with a concussion, carefully moving him aside, checking if there were any small fragments in his arms or legs, bandaging them, or applying a tourniquet if the bleeding was severe. Then I started doing more—I learned to apply splints, pack wounds, and bandage whatever injuries I could handle on my own.
You wait for the call and know there are wounded you can’t reach
Artem Koval, Combat medic, Volunteer Medical Battalion “Hospitallers”:
I joined the “Hospitallers” in the fall of 2023. It was the right decision for me. At that time, I was 19 years old. Before that, I had been a member of the Territorial Defense Forces, but since the Kyiv campaign had ended, I wanted to keep working. I decided to join the “Hospitallers” because they are not part of the Armed Forces—they are volunteers. You have enough free time to take care of your own things. When you’re mobilized, you’re fully tied up with service. Right now, my job is evacuating soldiers and civilians in front-line and near-front-line areas, handling everything from the ground up through different stages—medevac, casevac, and stabilization points.
Nonstop evacuation
I was 19 when I went on my first evacuation. There were three of us, and it was our first time on the front line.
Artem Koval
Combat medic, Volunteer Medical Battalion “Hospitallers”
We had just completed training with the “Hospitallers”—fresh off the course—and, roughly speaking, we were basically like little kittens. This was in Kherson. We were picking up guys being evacuated from Krynky, brought in by boat. They didn’t have severe injuries, but they were frostbitten and had concussions. Fortunately, they didn’t have any critical injuries.

Every day has its challenges. One such day was when we were evacuating a soldier and drove all the way to the very front-line positions—back then, you could still go to the “zero” line. You can’t do that now. The soldier had an open traumatic brain injury. We managed to evacuate him, but later, after surgery, I learned he had died. We did everything we could, but unfortunately, that’s how it goes sometimes.
There was one rotation when we evacuated 60–70 people in a single day. We just went nonstop. You arrive, load a couple of people into the vehicle, turn around, and drive off again.
Sometimes it’s calm. In a way, that’s good, because when there’s no work, you can rest.
But you still understand that just because there’s no work at the moment doesn’t mean there are no wounded. It only means I can’t go get them because the situation on the ground doesn’t allow it.
Artem Koval
Combat medic, Volunteer Medical Battalion “Hospitallers”
But I know there are wounded out there. There always are.
Different reality
Right now, the hardest thing for a combat medic is sitting still and not being able to evacuate a wounded person. You’re ready, fully prepared, but you have to stay put for a couple of hours, sometimes almost a whole day, because the situation doesn’t allow you to do anything. Once you get into the work, it’s great. I really don’t like riding in the vehicle when going on a mission—you can’t control the process. But as soon as a wounded person comes under my care, I understand that this is my responsibility. I’m in charge there; I manage the situation and take the lead.
People are often scared. They don’t know what will happen to them. They don’t know who you are. At a minimum, you need to earn their trust to show that you won’t harm them, and that you’re there to help. I try to exchange phone numbers with them so I can check in on them later.

The most difficult thing is seeing fallen soldiers—they are heroes—who have already given the most valuable thing they could give. You have to examine them, pack all their belongings into a bag, and seal it. You see their body, badly mutilated, and you realize that the family won’t get to say goodbye. The coffin won’t be opened because the body is completely disfigured. And you realize that you might be one of the last people to see them.
Emotions are a bit of a complicated issue for me. Over time, I’ve stopped really feeling them. I can calmly pack a person into a body bag without any emotion. I understand that this is the reality, and I entered it at a very young age. For me, it has simply become routine. Unfortunately, that’s the scariest part. I wouldn’t want it to be this way, but it happened.
There are very few people you can talk to about these situations. Your family can’t fully understand—they’re not part of this world, and they shouldn’t have to be. It’s enough that one person in the family is fully immersed in it, rather than the whole family being affected. Your loved ones live in a slightly different reality.
But I made my choice consciously. No one forced me. I’m still young. I think I’ll manage. I have my whole life ahead of me. I’m only 22—I still have a life to live. But I’m basically spending my youth at war. In 2014, when I was 11, I was drawing pictures for the ATO soldiers, and now I’m the one receiving those drawings from children.
I have been a war veteran since 2017. I am also a veteran of the Armed Forces. My military career began in the last century, and this year I will celebrate a milestone—30 years of continuous service. During the full-scale invasion, I served in combat as part of the 17th Brigade of the National Guard of Ukraine “Raid”, and currently serve in a rear support unit.
We can buy weapons, but our people cannot be replaced
Natalia Shtoka, Chief of the Medical Station, the 37th Regiment, National Guard of Ukraine:
I have been a war veteran since 2017. I am also a veteran of the Armed Forces. My military career began in the last century, and this year I will celebrate a milestone—30 years of continuous service. During the full-scale invasion, I served in combat as part of the 17th Brigade of the National Guard of Ukraine “Raid”, and currently serve in a rear support unit.
Family tradition
My family has a long military tradition. Generation after generation, we’ve served our country and defended our people. Even back in school, I was always part of the medical team and dreamed of becoming a military medic. I ran around with a little bag marked with a red cross and said that when I grew up, I would become a medic. By education, I am a feldsher. My job involves diagnostics, providing medical care, and directing patients to the right specialists. A significant part of my work is with service members after their injuries, supporting their treatment and rehabilitation.

In 2017, after returning from maternity leave, I went to the Anti-Terrorist Operation zone in Mariupol. After that, I served multiple rotations in the Donetsk region. Before Russia’s full-scale invasion began, I had already been actively involved, gained significant experience, and understood what was happening. Therefore, in May 2022, as a combat medic, I deployed to the Kharkiv region as part of a battalion of mobilized servicemembers.
The hardest thing for me was realizing that I might have to physically take people’s lives.
Natalia Shtoka
Chief of the Medical Station, the 37th Regiment, National Guard of Ukraine
I am a medic, and my whole life I have been saving people, whether they are soldiers or civilians. There were times when mothers with children came to us for help because we were the only medical personnel around who could at least make a diagnosis and provide basic medical care.
But in 2022, I had to pull the trigger. It was hard. Truly hard. It created a very deep sense of inner conflict for me.
Human force
At different periods, I had different responsibilities. When I was in the combat zone, the priority was saving the wounded. Since 2023, after sustaining an injury, I have gradually moved each year from the combat zone to rear positions. Now my main task is to organize proper medical care for everyone who needs it. In other words, we provide general medical care and refer patients for surgery, prosthetics, and rehabilitation.
Right now, in this position, being a military medic for me means saving our human force. Human force means our soldiers—the one asset that cannot be replenished.
We can buy weapons, we can buy missiles, but the human force—our people—cannot be replaced.
Natalia Shtoka
Chief of the Medical Station, the 37th Regiment, National Guard of Ukraine
We must preserve them, because they are the only thing that cannot be replenished.

We could hire mercenaries who would fight for money, but they would never have the same desire for freedom and independence as our people.
My main task now is caring for people’s health. Even elderly people can still do something and want to help. In 2022, I was in that environment and saw people’s patriotism, unity, support, and care for one another. We were like one big family.
People who have their own families have something to lose and something to protect. It is especially painful when young people die—particularly when a young man with no wife or children is killed, someone who has just finished school, left his family, his mother and father, and begun an independent life. They didn’t even have time to truly live it. That is deeply tragic.
We receive people who have already served in combat units and, due to their health condition, can no longer perform combat duties. However, they are still fit for service in rear support units. Together, we guard important state facilities and provide logistical and material support, thereby helping those on the front line.
Despite all this, my guys still go on rotations and continue to defend our Homeland.
You do everything to save them, even when it’s already too late
Vladyslav Chubenko, Head of Medical Supply of the Military Unit, 24th Separate Mechanized Brigade:
It was 2022. I was finishing medical college at the age of 19. At the TCC, they told me, “First, finish your studies, then you can sign a contract.” After graduating, I went back to my local recruitment office, but they still said, “Kid, you should go home.” So I enlisted through the regional military commissariat in August 2022.
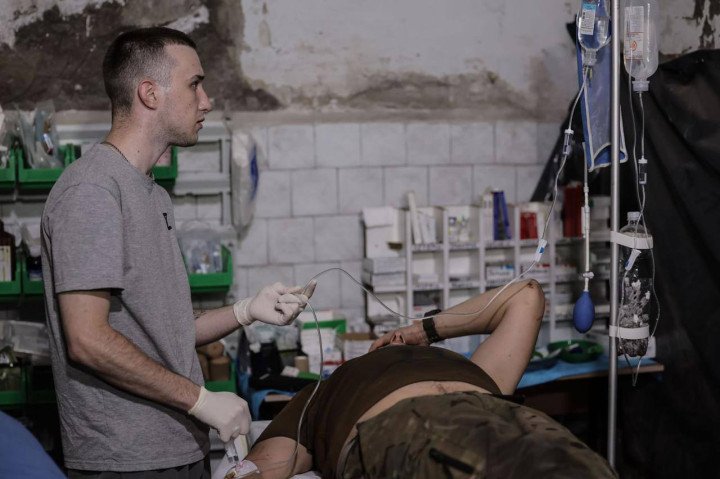
My mom and I even joked about who would gather the documents faster—her or me. I have a brother who is 10 years younger than me, and if it weren’t for him, maybe my mom and I would have gone to serve together. But someone had to stay with him, and at that time, my father was working with the fallen, so I helped him. Now we serve in the same brigade.
“I want to work”
I was assigned to the 24th Separate Mechanized Brigade. Initially, I served as a nurse. Later, I was promoted to medical instructor, then to a feldsher. Now, I serve as the head of the medical supply in a military unit.
At the end of 2022, we were stationed on the outskirts of Chasiv Yar. At first, they wouldn’t let me go on evacuations because I was only 19 and had just arrived at the unit. I would just watch the guys head out on 12-hour shifts, and I really wanted to go with them. I kept saying, “Let me go, I want to work.” Eventually, they started sending me out on evacuations. My first mission turned out to be quiet. That felt unusual to me. There were no wounded, no shelling.
At first, we were stationed at one location. Then cluster munitions from Russia’s Grad rockets started landing there. We kept changing our position—not too far, so the battalions would know where we were. I remember December 25th [2022—ed.] very clearly. It was a hard evening. I had fallen asleep in the vehicle and woke up to the engine starting and the car speeding off. I asked the driver what had happened, and he replied, “We couldn’t stop to offload the wounded. It’s critical. We can’t waste any time—we’re going straight to the stabilization point.”
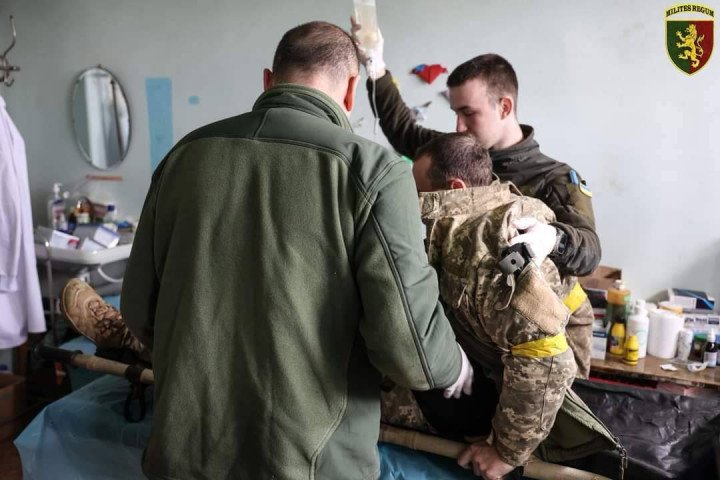
I said, “Okay, but what happened?” And he told me the whole story. He was standing there when a vehicle pulled up and started flashing its headlights, and right behind it—another one. A British journalist jumped out of the first car, grabbed my driver by the arm, and led him to the second vehicle.
Our driver said, “I opened the door—and they were all torn up, screaming. Some of them didn’t even have tourniquets.”
Vladyslav Chubenko
Head of Medical Supply of the Military Unit, 24th Separate Mechanized Brigade
He immediately applied tourniquets to everyone who needed them. Without even transferring them to our vehicle, they just followed right behind us. We reached the stabilization point and began working. I remember it vividly because it was my first real experience working with the most severe cases. But we managed—there were no losses. Later, I found out they were all okay. One of them did lose a lower limb to amputation, but he survived.
Dealing with loss
The hardest moments are when they bring someone in, and you understand—it’s over. But you still look at the doctor, and at that moment, we start resuscitation. Everyone starts working like bees.
Everyone knows their role—connecting equipment, starting CPR, intubation—doing everything possible to at least try to save them.
Vladyslav Chubenko
Head of Medical Supply of the Military Unit, 24th Separate Mechanized Brigade
At least to try. Yes, it may cost us time, but we’re there so they have hope—so they have a chance to survive.
I always tell the wounded: “We’re here for you. We’re here so that if you get injured, you’ll know we’re here, and we’ll help you. No matter what, we will help.”
The hardest thing is loss. Especially losing young guys. Even though we do everything possible to save them, sometimes it just doesn’t work. We’re not the Almighty— we can’t just save someone when it’s impossible. There’s apathy, there’s burnout. Sleep problems—sometimes you dream about a wounded person, someone you feel deeply sorry for. I’ve dreamed about the fallen. Sometimes you can’t fall asleep because you keep thinking about what you could have done better, what else might have been possible, what you could have done differently.
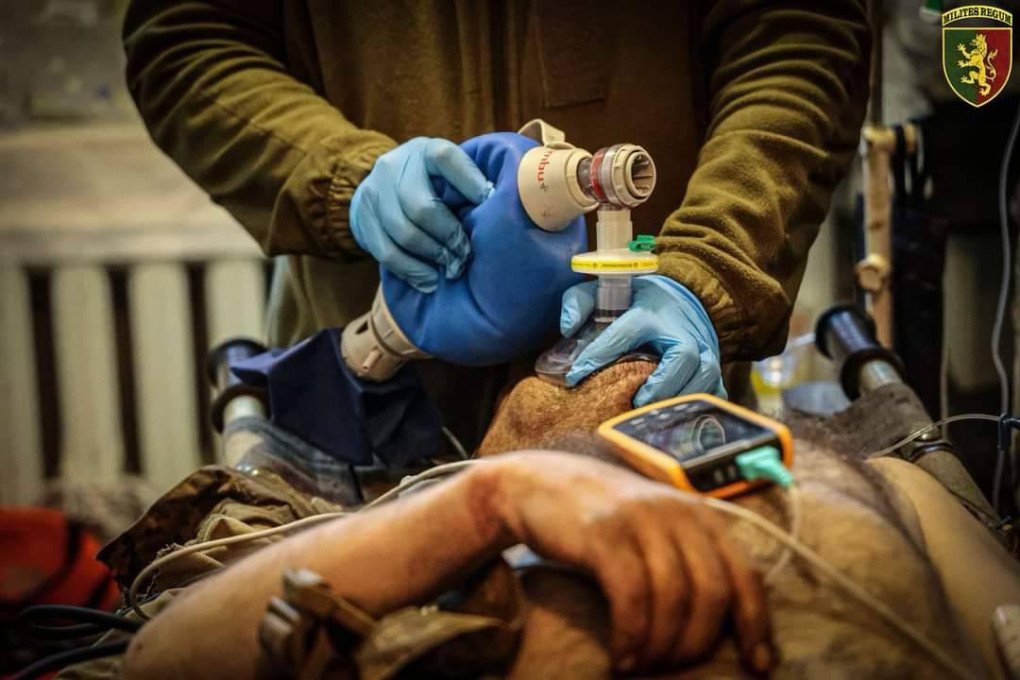
I’ve wanted to become a medic since I was a child. No one in my family has a medical education, but I always wanted to go into it. Even when I was in school, I knew I would study medicine. I’ve always liked studying. Before signing my contract with the Armed Forces, I enrolled in a bachelor’s program. I graduated with honors. I’m thinking about dedicating my life to psychology.
When I’m helping someone, I feel like I’m exactly where I’m supposed to be.
Discuss this article:
-9bd5e1532102621f8fb1c4ba871a3171.png)
-73e9c0fd8873a094288a7552f3ac2ab4.jpg)
-81b68be5e2d3df09acbb0e7274b75880.jpg)


-72b63a4e0c8c475ad81fe3eed3f63729.jpeg)


